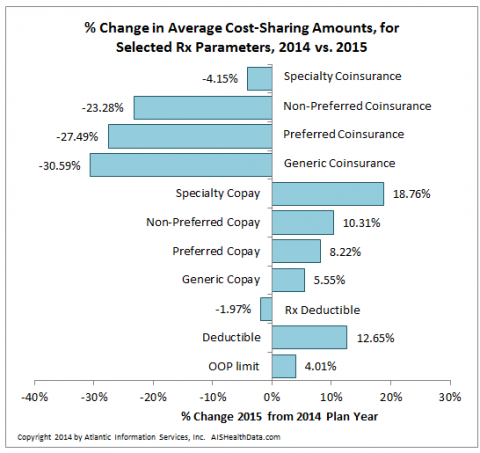
Health plans selling now for plan year 2015 are more likely to require a percentage-based coinsurance, versus a set copay amount for Rx fills, than they were in 2014. For specialty drugs, 23% more plans are charging a coinsurance than did so in 2014, for in-network retail fills.
However, the actual percentage of coinsurance required is lower at all formulary tiers compared to 2014. For set copay amounts, though, the cost-share amount is up — 5.55% for generics and almost 19% for specialty drugs.
Average copays per formulary tier for this sample of 2015 plans are $11.15 for generics, $42.14 for preferred brand drugs, $77.45 for non-preferred drugs and $143.22 for specialty drugs. Where coinsurance is applied, average percentages are 13.8% for generics, 17.16% for brand preferred, 22.37% for non-preferred and 25.59% for specialty.
The data set RxB used for this analysis represents 118 MCOs and 39 states for which data was available in both 2014 and 2015. The 2014 sample included 7,265 plans, and the 2015 sample includes 6,669 plans. All cost-sharing data in this analysis is for in-network retail pharmacies. AIS will upload new plans to the data set as soon as possible, and subscribers will receive an email notification.